Understanding Castleman Disease: A Complex Immune Challenge
Castleman disease (CD) represents a unique group of rare and often perplexing disorders that fundamentally involve the lymph nodes, crucial components of our immune system. While it's characterized by enlarged lymph nodes and a spectrum of inflammatory symptoms, its rarity and the variability of its presentation make accurate diagnosis a significant challenge. For those grappling with unexplained inflammation, persistent fatigue, or swollen lymph nodes, understanding the definitive diagnostic pathway for Castleman Disease: Understanding This Rare Lymph Node Disorder is paramount. The cornerstone of this pathway, as we will explore, is the indispensable lymph node biopsy.
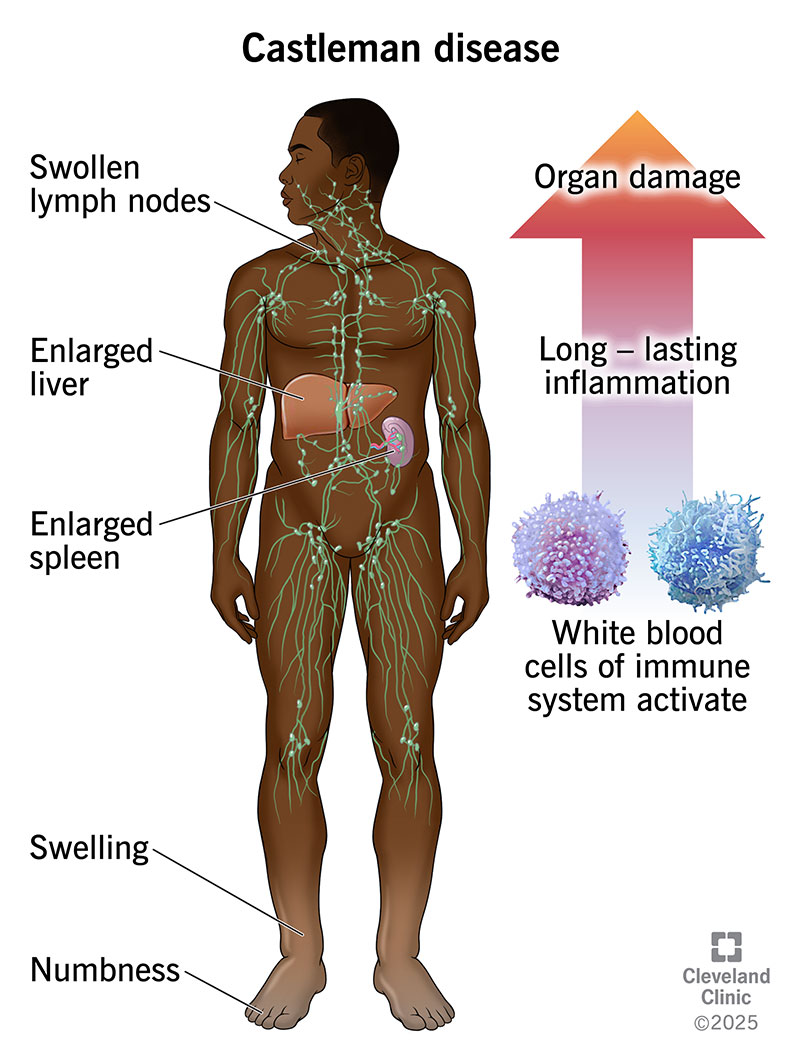
At its core, Castleman disease occurs when lymph nodes undergo an abnormal transformation. For reasons not yet fully understood, these nodes, normally vigilant against invading organisms, begin to overproduce lymphocytes and various inflammatory compounds. This uncontrolled proliferation leads to the characteristic lymph node enlargement and can trigger systemic inflammation, potentially impacting multiple organs and causing a wide range of debilitating symptoms. The intricate nature of CD means that while many conditions can cause swollen glands, identifying the specific microscopic changes associated with Castleman disease requires a precise and definitive diagnostic tool.
The Diagnostic Maze: Why Castleman Disease is So Hard to Pinpoint
One of the primary difficulties in diagnosing Castleman disease stems from its masterful ability to mimic other illnesses. Patients often present with a broad array of non-specific symptoms and laboratory abnormalities that could point to numerous other conditions, from autoimmune disorders and infections to various cancers. Common symptoms like persistent fever, night sweats, weight loss, fatigue, and, of course, enlarged lymph nodes, are not unique to CD. This symptomatic overlap creates a diagnostic "maze" for clinicians, where initial investigations may not immediately zero in on Castleman disease.
Consider a patient experiencing unexplained weight loss and swollen glands. These symptoms could suggest lymphoma, tuberculosis, HIV, or an autoimmune disease like lupus. Without a specific and definitive test, a precise diagnosis of Castleman disease can be delayed, sometimes for years, leading to prolonged suffering and potentially inappropriate treatments. The heterogeneity of CD's presentation – meaning symptoms can vary wildly even within the same subtype – further complicates matters. This chameleon-like nature underscores why relying solely on clinical symptoms or routine blood tests is insufficient for a conclusive diagnosis and highlights the critical need for a more direct, microscopic examination of the affected tissue.
The Lymph Node Biopsy: The Cornerstone of Castleman Disease Diagnosis
Given the diagnostic complexities, the lymph node biopsy emerges as the single most critical step in confirming Castleman Disease. It's not just another test; it's the definitive procedure that provides the irrefutable evidence needed for an accurate diagnosis. This isn't a simple blood draw; it involves the surgical removal of an entire enlarged lymph node, or at least a significant portion via an excisional or core needle biopsy, for detailed examination.
What Happens During a Biopsy and Pathology Analysis?
Once the enlarged lymph node is obtained, it is meticulously processed and analyzed by a specialized pathologist. This expert uses a light microscope to search for very specific, hallmark microscopic features unique to Castleman disease. These features include particular patterns of cellular organization, follicle regression, vascular proliferation, and other histological changes that differentiate CD from other conditions that might cause lymph node enlargement. It's a highly specialized analysis that requires an experienced eye trained in recognizing the subtle but crucial characteristics of this rare disorder.
The pathologist’s role is invaluable. They don't just confirm enlargement; they scrutinize the internal architecture of the node. They look for specific changes such as "lollipop lesions" (lymphoid follicles with a penetrating vessel) or concentric layering of lymphocytes around germinal centers. These unique microscopic signatures are what finally unlock the diagnosis of Castleman disease, distinguishing it from look-alike conditions.
Preventing Misdiagnosis: The Biopsy's Critical Role
The requirement for a lymph node biopsy and subsequent expert pathological analysis is absolutely vital to prevent misdiagnosis. Without it, patients with other diseases that present with similar symptoms and enlarged lymph nodes could be incorrectly diagnosed with Castleman disease, leading to inappropriate and potentially harmful treatments. Conversely, genuine CD patients might be misdiagnosed with more common conditions, delaying the specific care they truly need. The biopsy acts as a safeguard, ensuring that the patient receives the correct diagnosis, which in turn dictates the most effective treatment strategy and improves prognostic outcomes.
Unlocking Subtypes: How Biopsy Guides Treatment Pathways
Beyond simply confirming the presence of Castleman disease, the lymph node biopsy plays an equally critical role in differentiating between its various subtypes. This distinction is not merely academic; it has profound implications for treatment strategies and patient prognosis. There are several main subtypes, broadly categorized into Unicentric Castleman Disease (UCD) and Multicentric Castleman Disease (MCD), with further distinctions within MCD.
- Unicentric Castleman Disease (UCD): Involves a single enlarged lymph node or a single region of enlarged nodes. Patients often experience localized discomfort, and crucially, surgical removal of the affected node frequently leads to a complete resolution of symptoms and no further complications.
- Multicentric Castleman Disease (MCD): Characterized by multiple enlarged lymph nodes and systemic inflammation that can affect various organ systems. MCD itself is further categorized into:
- HHV-8-associated MCD (HHV-8+ MCD): Caused by Human Herpesvirus-8 infection.
- HHV-8-negative/Idiopathic MCD (iMCD): Occurs for unknown reasons.
- POEMS-associated MCD and Oligocentric CD: Other distinct subtypes with specific clinical presentations.
The pathologist's analysis of the biopsy specimen helps pinpoint these specific subtypes, as microscopic features, while sharing commonalities, can also differ greatly between them. For instance, the presence of specific cell types or viral markers (like HHV-8) within the lymph node tissue helps guide this critical differentiation. For a more detailed understanding of these distinctions, you can read UCD vs MCD: Decoding Castleman Disease Subtypes and Their Impact.
Why is this distinction so vital? Because UCD, HHV-8+ MCD, and iMCD can have vastly different symptoms, require different treatment approaches (ranging from surgery for UCD to targeted immunotherapies for MCD), and carry distinct prognoses. An accurate subtyping through biopsy ensures that patients receive the most appropriate and effective care tailored to their specific form of Castleman disease, significantly improving their chances of a positive outcome.
Beyond the Biopsy: Advocating for an Accurate Castleman Disease Diagnosis
For patients and caregivers, navigating the diagnostic journey for a rare disease like Castleman disease can be daunting. While the biopsy is key, several practical tips can empower you:
- Be Your Own Advocate: If you or a loved one experiences persistent, unexplained symptoms, particularly enlarged lymph nodes, and previous tests have been inconclusive, don't hesitate to ask your doctor about the possibility of Castleman disease and the necessity of a lymph node biopsy.
- Seek Specialized Care: Due to its rarity, not all doctors may be familiar with Castleman disease. Request a referral to specialists such as hematologists, oncologists, or immunologists who have experience with lymphoproliferative disorders.
- Consider a Second Opinion: Especially for pathology results, a second opinion from a pathologist specializing in rare lymph node disorders can be invaluable in confirming a complex diagnosis like Castleman disease.
- Document Everything: Keep a detailed record of symptoms, their duration, previous tests, and treatments. This comprehensive history can provide crucial clues for your medical team.
Conclusion
Castleman disease, with its multifaceted presentation and elusive nature, poses a formidable diagnostic challenge. While its symptoms can mirror numerous other conditions, the unwavering truth remains: a definitive diagnosis hinges on a lymph node biopsy. This crucial procedure, followed by meticulous pathological analysis, not only confirms the presence of Castleman disease but also precisely identifies its subtype, directly guiding tailored treatment strategies and ultimately improving patient outcomes. For anyone navigating the complex world of unexplained lymph node enlargement and systemic inflammation, understanding the pivotal role of the biopsy is the first critical step toward an accurate diagnosis and effective management of Castleman Disease.